Neat Little Guide — 13 minutes
Allergies impact your health
What is an allergy?
Our body fights any external enemy (e.g., microbe, virus, bacterium or parasite) with a very powerful weapon: the immune system. When this “weapon” considers a substance (allergen) that has been eaten, drunk, breathed or touched as a serious enemy, it overreacts by producing a particular type of antibody called “IgE” (immunoglobulin E) to fight it. This is the allergic reaction.
An allergy, also known as “type 1 hypersensitivity,” can manifest itself in different parts of the body such as the skin, eyes, digestive system or respiratory tract. The type of symptoms and their intensity, which depend on several factors, are specific to each person. Allergic reactions can be subtle, such as skin redness, or potentially life-threatening, such as anaphylaxis.
Allergies should not be confused with intolerance. If a reaction is not caused by IgE antibodies, it is not an allergy. Rather, it is referred to as intolerance, as in cases of “gluten intolerance” or “lactose intolerance.” For example, celiac disease, the most serious form of gluten intolerance, is the result of an inflammation of the intestine caused by immunoglobulins of type G (IgG) and type A (IgA), antibodies that are different from IgE. Therefore, the condition does not have the same mainly digestive symptoms and, above all, does not carry any risk of an anaphylactic reaction. Lactose intolerance is not caused by antibodies, but by a lack of lactase, the enzyme in the small intestine responsible for digesting lactose (the sugar present in dairy products).
Read more: Food intolerance or allergy? They are often confused, but they are very different.
Quick appointment and results. Screening of more than 650 allergens.
What causes allergies?
Some of the most common allergens include the following:
| Airborne allergens | Food allergens | Other allergens |
|---|---|---|
| Tree, grass and ragweed pollens | Peanuts | Some medications (e.g., penicillin) |
| Dust mites | Cow’s milk | Latex |
| Animal hair, urine, saliva and dandruff | Eggs | Insect venom |
| Mildew | Nuts | |
| Seafood | ||
| Fish | ||
| Sesame |
Although they are not the most common, food allergies have generated a great deal of interest due to their increasing prevalence. About 4% of the Quebec population has a food allergy. According to the province’s Ministère de la Santé et des Services sociaux, 6% of babies and 3% of children aged 10 or older have a food allergy, compared to only 1% to 2% of adults.
The most common cause of an allergy in toddlers is milk. Fortunately, this allergy disappears in 76% of cases before the age of five. In fact, most children see their food allergies (milk, eggs, soy) disappear before the age of seven, including peanut allergies in 20% of cases. It should be noted that 10 foods are responsible for more than 90% of allergic reactions and must be included in the list of ingredients of products sold in Canada: cow’s milk, eggs, peanuts, nuts (walnuts, hazelnuts, almonds, cashews, pecans and pistachios), fish, seafood, sesame, mustard, soy and wheat. These last two foods must be declared, but are rarely responsible for an IgE-mediated allergic reaction.
Allergic reactions can have minimal to very serious consequences
Allergic reactions can occur at any age, but are more common in children. The genetic predisposition to develop an allergy is called “atopy.” An atopic child may experience symptoms from birth in the form of skin reactions such as eczema, respiratory symptoms, nasal discharge (rhinitis) or other symptoms. Some symptoms may decrease or even disappear over time, while others tend to worsen over the years (asthma, anaphylaxis).
It should be noted that some atopic individuals will never have allergic reactions. They may have positive results to skin allergy tests even if they have no symptoms. In such cases, they are deemed to be “sensitive” to certain allergens and only a fraction of these people will ever have a severe allergic reaction. A British study found that barely a quarter of children sensitive to peanuts are at risk of having a major allergic reaction. [1]
An allergic reaction generally occurs in two phases:
Sensitization: Sensitization occurs when an allergen first comes into contact with the body through the skin or mucous membranes (eyes, respiratory tract or digestive tract). Sometimes, exposure to the allergen occurs through the components of breast milk or, more frequently, through skin contact. Most often, the immune system becomes “tolerant,” meaning that it gets accustomed to the allergen and no longer reacts to its presence. Otherwise, it can react by classifying the foreign substance as dangerous. Therefore, it will keep a “memory” of the recipe for producing antibodies in case the allergen shows up again. This sensitization phase is asymptomatic, meaning that no symptoms are present.
Allergic reaction: This occurs upon subsequent contact with an allergen, when the immune system is ready to react. Antibodies (IgE) on the surface of some white blood cells (mast cells) seek to destroy the allergen by triggering a series of defensive reactions. Mast cells are rich in histamine and other chemicals that, once released, cause allergy symptoms. This is why antihistamines are often used to relieve minor allergy symptoms.
Anaphylaxis is the most severe form of allergic reaction. It is sudden, widespread and, if not treated promptly, can progress within minutes to anaphylactic shock, a sudden drop in blood pressure that can result in a loss of consciousness or death. The first signs of an anaphylactic reaction are the following:
- Skin (cutaneous system): Presence of a rash, swelling, itching, heat sensation, redness or cutaneous eruption
- Upper respiratory tract: Sneezing, runny nose, red eyes, swelling of the lips, difficulty speaking or swallowing and hoarse voice
- Lower respiratory tract: Difficulty breathing, coughing, wheezing, shortness of breath, chest pain or tightness
- Digestive system: Nausea, abdominal pain or cramps, vomiting and diarrhea
The cardiovascular system may also be affected (pale or bluish complexion, weak pulse, loss of consciousness, dizziness, vertigo or shock). The individual may even have anxiety, a feeling of “imminent danger,” headaches or a metallic taste in the mouth.
Increasingly frequent reactions
Worldwide, the prevalence of allergic diseases has doubled over the past 30 years. Nearly 40% of the population in industrialized countries is affected by some form of allergy.
By observing social and environmental changes, several experts and researchers have proposed hypotheses that may explain why allergies have increased.
The hygienic hypothesis: We are too clean!
At home, at work or during our leisure time, we live in an increasingly sanitized environment. Powerful disinfectants remove agents that stimulate our immune system, thereby reducing its ability to fight the allergens it encounters.
Some experts claim that, to have a strong and healthy immune system, we need to be in contact from an early age with viruses and bacteria that allow it to develop. This is why children who have four or five colds a year are less likely to have allergies.
Climate Change – A major impact on Allergic Rhinitis
According to Quebec’s ministère de la Santé et des Services sociaux (MSSS), the increase in greenhouse gases and the resulting climatic conditions, such as rising temperatures and humidity, affect allergenic plants as follows:
- Longer growing season
- Spread of some species to new areas
- Increased pollen production
- Increase in the allergenic potential of pollen
For example, the MSSS states that the length of the pollen season in Montreal increased by 33% between 1994 and 2002, going from 42 to 63 days. What’s more, the daily averages for pollen concentrations, which were 36.3 grains of pollen per cubic metre in 1997, almost doubled to 68.8 grains of pollen per cubic metre in 2002.
Therefore, climate change can have an impact on human health by increasing the frequency and severity of respiratory allergy episodes (rhinitis, conjunctivitis and asthma).
Read more: Some people can actually be clinically allergic to exercise
Allergy diagnosis
The diagnosis of an allergy must be made by an allergist, a health care professional specialized in this field. Although some allergies are easier to diagnose, the very large number of potentially allergenic agents, especially in the environment and in food, the possibility of cross-allergies and allergy combinations such as pollen-food syndrome or the existence of true multi-allergies, make some diagnoses particularly complex.
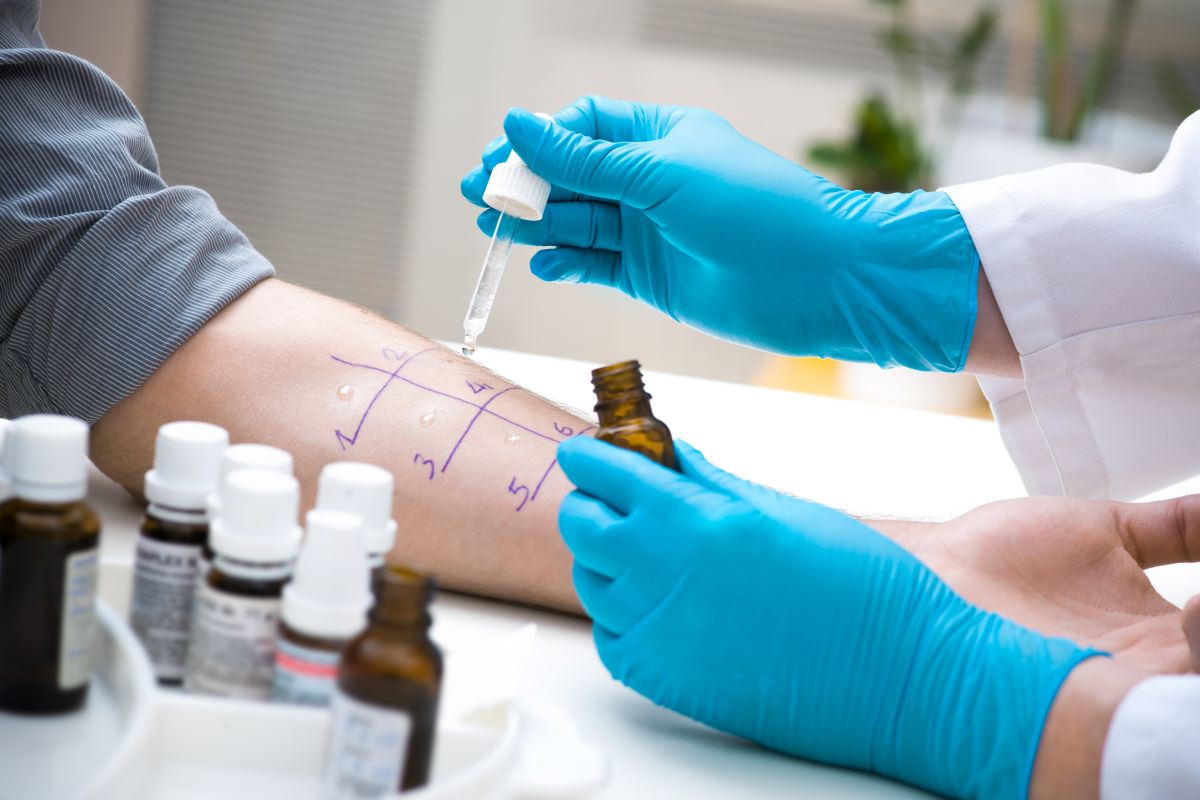
Therefore, any allergy diagnosis is based above all on detailed observation. The type of symptoms and the circumstances of the reaction will enable the specialist to determine the appropriate tests: a combination of skin tests and blood IgE assays. The skin test involves applying small amounts of extracts of the suspected allergen (peanut extract, milk extract, animal allergens, pollen, etc.) to the skin of the arm to study the cutaneous reactions. Blood IgE assays involve bringing a drop of blood into contact with the same raw extracts of the suspected substances to detect the presence of specific IgE antibodies.
In some cases, a definitive diagnosis of an allergy (or the absence of an allergy) can only be based on provocation testing, which involves administering a preparation of a suspected allergen orally (food allergy) or by inhalation (respiratory allergy). Since some individuals may experience symptoms as severe as anaphylaxis, it goes without saying that these tests can only be performed by experienced personnel in well-equipped clinics.
Molecular allergens
For several years, allergy specialists have had an additional tool at their disposal to diagnose and possibly treat allergies: molecular allergens, or pure allergenic components. In the case of a peanut allergy, skin or blood tests have always been performed with raw peanut extracts containing dozens or even hundreds of potentially allergenic components. Research conducted in recent years has made it possible to isolate and manufacture in the laboratory the most suspicious components of the peanut, which are called “rAra h1,” “rAra h2,” and so on.
Therefore, it is now possible to search for specific IgE antibodies that react to each of these pure components. This is how it was discovered that the majority of children allergic to peanuts had rAra h1, rAra h2 or rAra h3 IgE antibodies in their blood, while children who were sensitive but not allergic to peanuts did not have these IgE antibodies but rather other types of IgE antibodies such as rAra h8 (cross-reactive with a protein also found in birch pollen) or rAra h9 antibodies.
Allergy treatment
Most people know that symptoms of a seasonal allergy can be relieved by taking antihistamines or nasal corticosteroids. Asthma symptoms can also be relieved with a bronchodilator and corticosteroid pump. There is also a sublingual desensitization treatment in tablet form to treat rhinoconjunctivitis caused by dust mites, grass pollen and ragweed.
In the case of food allergies or insect venom allergies, the importance of an epinephrine auto-injector (EpiPen®) is well established: it must be used quickly as it is the treatment of choice and can save lives in cases of anaphylaxis.Over the years, other medications have been added to the kit to reduce the severity of an allergic reaction. Recently, dupilumab (Dupixent) and omalizumab (Xolair) have been used to treat more severe cases of eczema, hives or asthma. These very useful, even essential, drugs do not, however, cure allergies. In the case of food allergies, it is obviously possible to avoid eating a particular food, but it is much easier said than done!
To cure an allergy, the immune system needs to be re-educated so that it stops considering an allergen as an enemy molecule that it must eliminate. For environmental allergens such as pollen, dust mites and insect venom, this desensitization is achieved by injecting ever-increasing doses of the allergen under the skin. Desensitization occurs over a period of at least three years (or more, especially in the case of venom). In some cases, molecular allergens could reduce the duration of the treatment.
For food allergies, oral desensitization is the most innovative treatment. Inspired by subcutaneous treatment, it involves administering increasing doses of the allergen, this time by mouth.
In 2018, the first oral immunotherapy clinic in Quebec opened its doors at Montreal’s Sainte-Justine Hospital and has been a resounding success … with a long waiting list..[3] In response to this enthusiasm, the Montreal Children’s Hospital followed suit by also offering this innovative but difficult-to-access method.
With respect to allergy prevention, another new idea is gaining ground: instead of delaying the introduction of certain foods to infants, it is proposed to introduce potentially allergenic foods at an earlier age, meaning around four to six months for peanuts (provided that the texture of the preparation is suitable for the age to avoid any risk of choking).[4]
Conclusion
From the early introduction of allergenic foods to sublingual desensitization, the impending development of a vaccine [2] and the increasing accessibility of molecular allergens to detect and treat allergies, this vast field of medicine is constantly evolving. Breakthroughs in research are promising and expected to rapidly reduce allergic problems in a large number of individuals.
This text was written with the assistance of:
Marie-Josée Francœur, MD
Pediatric Allergist Specialist Clinic – DIX30 Medical Clinic / Head of Allergy department, CISSS Montérégie – Hôpital Charles-LeMoyne
Sources4
- N. Nicolaou et al., “Allergy or tolerance in children sensitized to peanut: prevalence and differentiation using component-resolved diagnostics,” Clinical Immunology [online], vol. 125, no 1, January 2010, p. 191-197.e13, https://www.ncbi.nlm.nih.gov/pubmed/20109746 (consulted on May 28, 2019)
- Binh An Vu Van, “Allergies : bientôt un vaccin?,” Québec Science [online], July 21, 2015, https://www.quebecscience.qc.ca/sante/allergies-bientot-un-vaccin/ (consulted on May 28, 2019)
- Philippe Mercure, “Allergies alimentaires : Affronter le mal au lieu de l’éviter,” La Presse Plus [online], March 24, 2019, http://plus.lapresse.ca/screens/b6885937-f140-47ca-a546-8b11025b31e5__7C___0.html (consulted on May 28, 2019)
- Benetta Chin et al. “Exposition précoce aux aliments et allergies alimentaires chez les enfants,” Le Médecin de famille canadien [online], vol. 60, no 4, April 1, 2014, p. e208-e210, https://www.cfp.ca/content/60/4/e208 (consulted on May 28, 2019)
